A growing number of services now offer “bone health” scans — but different tests measure different things. DXA, TBS, VFA, REMS and heel ultrasound are not interchangeable. Understanding what each one does (and does not) tell you is essential to making meaningful clinical decisions.
By Dr Taher Mahmud FRCP
Consultant Rheumatologist & Co-Founder, London Osteoporosis Clinic
Updated: May 2026
Key Takeaways
- No single test tells the full story of bone health — fracture risk depends on bone density, bone quality, clinical history, and lifestyle factors together.
- DXA scanning remains the gold standard for diagnosing osteoporosis and generating T-scores and Z-scores.
- TBS adds information about bone microarchitecture that DXA alone cannot capture — two patients with identical T-scores may have meaningfully different fracture risks.
- VFA (Vertebral Fracture Assessment) detects silent vertebral fractures that are frequently missed without specific imaging.
- High-street heel ultrasound scans are useful screening prompts but cannot diagnose osteoporosis or replace DXA.
- Blood tests help identify why bone is being lost — a critical step before deciding on treatment.
Why Can’t One Test Tell You Everything About Your Bones?
Many people understandably assume that a single scan — any scan — can definitively determine whether their bones are healthy. In reality, different tests measure different aspects of bone strength, bone quality and fracture risk.
Some tests are diagnostic. Some are supportive. Some are useful primarily as a screening prompt to seek a more formal assessment.
The important question is never simply “What does the scan show?” but rather “What does the result actually mean in context?”
In clinical practice, fracture risk is shaped by several interacting factors: bone mineral density, bone microarchitecture and quality, previous fracture history, clinical risk factors, falls risk, and the rate of ongoing bone loss. Two people can have identical DXA results yet carry very different fracture risks.
This is why a useful analogy is cardiovascular medicine: assessing bone health using only bone density is a little like assessing heart disease risk using blood pressure alone — informative, but incomplete.
What Does a Structured Bone Health Assessment Include?
At the London Osteoporosis Clinic, bone health assessment uses a structured, multi-layered framework. Each layer adds information the previous one cannot provide. The key principle is this: DXA remains the gold standard for diagnosing osteoporosis, but bone health assessment should not stop at DXA alone.
Tier 1 — Clinical Assessment
The most informative part of osteoporosis care is often not the scan itself, but the clinical consultation surrounding it. A structured assessment looks for factors that independently elevate fracture risk, including:
- Family history of osteoporosis or hip fracture
- Previous fragility fracture (fracture after minimal trauma)
- Long-term corticosteroid use
- Inflammatory conditions such as rheumatoid arthritis or inflammatory bowel disease
- Early menopause, low body weight, or history of amenorrhoea
- Excessive alcohol consumption or current smoking
- Falls risk — balance, strength, medications, and environmental factors
The FRAX calculator integrates these factors to estimate 10-year fracture probability and is widely used internationally. However, FRAX is a guide rather than a complete answer — it does not fully capture trabecular bone quality, silent vertebral fractures, treatment response, or falls risk in detail.
Tier 2 — What Can Blood Tests Tell Us About Bone Loss?
Blood tests help identify why bone is being lost — which is critical before making treatment decisions. A laboratory evaluation may include:
- Calcium, phosphate, and alkaline phosphatase
- Vitamin D (25-hydroxyvitamin D)
- Parathyroid hormone (PTH)
- Thyroid function (TSH)
- Renal and liver function
- Sex hormones where clinically indicated
- Bone turnover markers (P1NP and CTX) — to assess the rate of bone remodelling and monitor treatment response
- Full blood count, ESR and CRP where secondary causes are suspected
A significant proportion of osteoporosis is secondary to potentially treatable underlying conditions — vitamin D deficiency, hyperparathyroidism, thyroid dysfunction, coeliac disease, and others. Identifying these drivers can materially change management.
Tier 3 — What Does a DXA Scan Actually Measure?
DXA (dual-energy X-ray absorptiometry) is the international reference standard for diagnosing osteoporosis. It measures bone mineral density at the spine and hips and generates:
- T-score — bone density compared with a healthy young adult reference population (osteoporosis is defined as T-score ≤ −2.5)
- Z-score — bone density compared with people of a similar age and sex (useful for identifying secondary causes in younger patients)
DXA is also the standard used in most fracture-risk algorithms, treatment thresholds, and major clinical trials. It uses minimal ionising radiation and typically takes 10–15 minutes.
What Is TBS — and Why Does Bone Quality Matter Beyond Density?
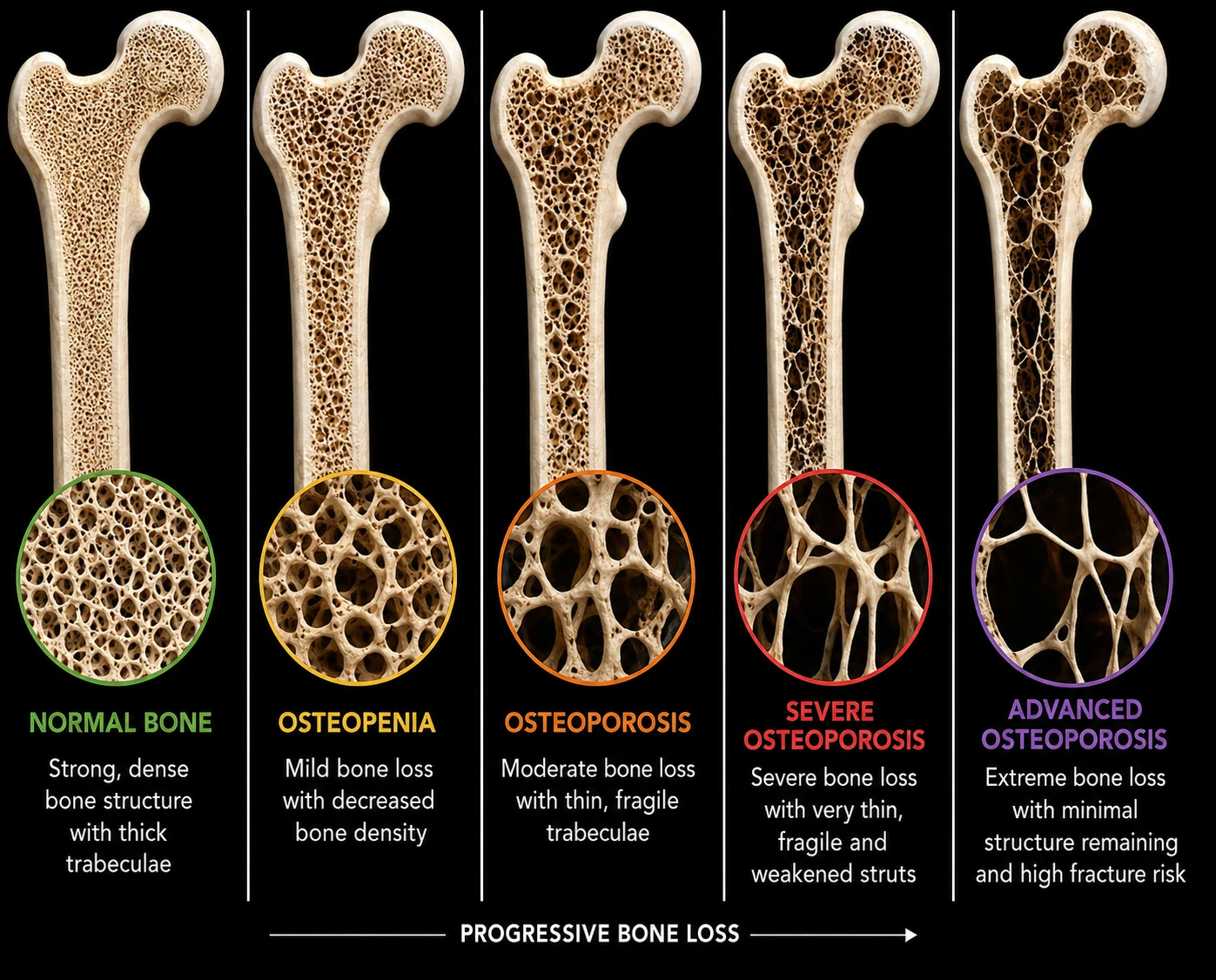
TBS (Trabecular Bone Score) is an advanced software analysis derived from the spine DXA image. It provides additional information about trabecular bone microarchitecture — effectively assessing aspects of bone quality, not simply density.
Two patients may have identical T-scores but meaningfully different TBS values and therefore different fracture risks. TBS has been validated in multiple clinical studies and is increasingly incorporated into fracture-risk algorithms alongside FRAX.
At the London Osteoporosis Clinic, TBS is routinely included as part of the full DXA assessment.
What Is VFA — and Why Are Silent Vertebral Fractures So Commonly Missed?
VFA (Vertebral Fracture Assessment) is a low-dose spinal image performed during the DXA appointment. It allows assessment of vertebral morphology to detect existing vertebral fractures.
Vertebral fractures are among the most common osteoporotic fractures — and they are frequently missed. Many occur without dramatic pain or obvious symptoms. A patient may sustain one or more vertebral fractures without ever presenting to their GP.
Detecting an existing vertebral fracture significantly changes fracture-risk categorisation and may alter treatment decisions. Importantly, some patients sustain fragility fractures despite bone density values outside the osteoporotic range — which is one reason why bone health assessment should never rely on a single number alone.
Tier 4 — What Is REMS and How Does It Compare With DXA?
REMS (Radiofrequency Echographic Multi-Spectrometry) is an ultrasound-based technology that estimates bone density without ionising radiation. It has accumulated increasing validation in clinical studies and may have a useful role where:
- Radiation exposure is a specific concern
- DXA access is limited
- Monitoring is required at intervals closer than standard DXA scheduling
REMS is best viewed as a complementary tool rather than a replacement for DXA at present. DXA remains the current reference standard for diagnosis and treatment threshold decisions.
Are High-Street Bone Scans Reliable?
Heel ultrasound scans — often called QUS (Quantitative Ultrasound) scans — are widely available and can be a useful early screening prompt. They are non-invasive, involve no radiation, and are accessible outside specialist settings.
However, they are not equivalent to DXA. They do not directly measure spine or hip bone density, cannot formally diagnose osteoporosis, and should not be used alone to make treatment decisions. Their value lies primarily in identifying people who may benefit from a more comprehensive assessment — and prompting onward referral when results are concerning.
How Does LOC Bring All of This Together?
A T-score answers one question. Clinical decision-making requires a broader view.
At the London Osteoporosis Clinic, findings from clinical history, laboratory assessment, DXA, TBS, VFA and functional risk assessment are interpreted together to help patients understand:
- Where their bone density currently sits
- The likely trajectory of bone change if untreated
- Their 10-year fracture risk, incorporating all available information
- What treatment options are appropriate and what response is realistic
The goal is not simply to generate numbers, but to provide meaningful interpretation and a clear, personalised plan. If you would like to understand your bone health in this way, our consultant-led bone health assessment offers exactly that approach.
Who Should Consider a Bone Health Assessment?
A structured bone health assessment may be appropriate if you:
- Are a woman who has gone through the menopause, particularly in the first 5–10 years
- Are a man over 50 with additional risk factors
- Have had a fracture after a minor fall or minimal trauma
- Have been on long-term corticosteroids or other bone-affecting medications
- Have an inflammatory condition such as rheumatoid arthritis, IBD or coeliac disease
- Have a family history of osteoporosis or hip fracture
- Have noticed height loss, postural change, or persistent back pain
- Have had a heel ultrasound scan with a concerning result
The Bone Pathway™ at the London Osteoporosis Clinic combines consultant assessment, advanced imaging, laboratory evaluation and personalised management planning — with the aim of helping patients understand their bone health and long-term options.
The LOC View
The conversation about bone health in the UK has improved — more people know what a DXA scan is, and more are asking about it. But the clinical challenge I see daily is not just access to scanning; it is interpretation. A T-score is a starting point, not a conclusion. The patients who benefit most are those whose result is placed in the context of their full clinical picture — their history, their blood tests, their bone quality, their fracture risk, and their treatment options. That is what a consultant-led assessment provides that a scan alone cannot.
— Dr Taher Mahmud FRCP, Consultant Rheumatologist, London Osteoporosis Clinic
Frequently Asked Questions
What is the most accurate test for osteoporosis?
A DXA scan of the spine and hips remains the gold standard for diagnosing osteoporosis, particularly when combined with TBS and VFA where appropriate.
Is a DXA scan the same as a bone density scan?
Yes. DXA (sometimes written DEXA) is the technology used in standard bone density scanning.
What do T-score and Z-score mean?
The T-score compares your bone density with a healthy young adult reference population. The Z-score compares your bone density with people of a similar age and sex. A T-score of −2.5 or below meets the diagnostic threshold for osteoporosis.
What is TBS and why does it matter?
TBS (Trabecular Bone Score) provides additional information about bone microarchitecture and fracture risk beyond standard bone density measurements. Two patients can have the same T-score but different TBS values and meaningfully different fracture risks.
How does REMS compare with DXA?
REMS is an ultrasound-based technology with growing evidence supporting its use. DXA remains the current reference standard for diagnosis and treatment threshold decisions.
Are high-street bone scans reliable?
High-street heel ultrasound scans are useful screening tools but are not equivalent to DXA and cannot independently diagnose osteoporosis or guide treatment decisions.
Can you have osteoporosis with a normal DXA scan?
Yes. Some patients sustain fragility fractures despite bone density values outside the osteoporotic range. Bone quality, silent vertebral fractures, and falls risk all contribute independently to fracture risk.
How often should a DXA scan be repeated?
This depends on baseline results, treatment status, and individual risk factors. Your clinician will advise on appropriate timing — typically every 1–2 years on treatment, or every 2–5 years for monitoring.
Taking the Next Step
If you have had a heel scan with a concerning result, have recognised risk factors, or simply want a complete picture of your bone health, a structured consultant assessment is the most informative next step. The Bone Pathway™ at the London Osteoporosis Clinic provides exactly that — a multi-layered assessment interpreted in full clinical context.
Book a bone health assessment →
This article is intended as general information only and does not replace individual medical assessment. If you have concerns about your bone health, please consult a qualified clinician.
Dr Taher Mahmud FRCP is a Consultant Rheumatologist and Co-Founder of the London Osteoporosis Clinic, based at The Shard, London SE1. He holds two US patents in osteoporosis reversal and prevention and is a Trustee of the Global Osteoporosis Foundation.
Medically reviewed by Dr Taher Mahmud FRCP | Last updated: May 2026

